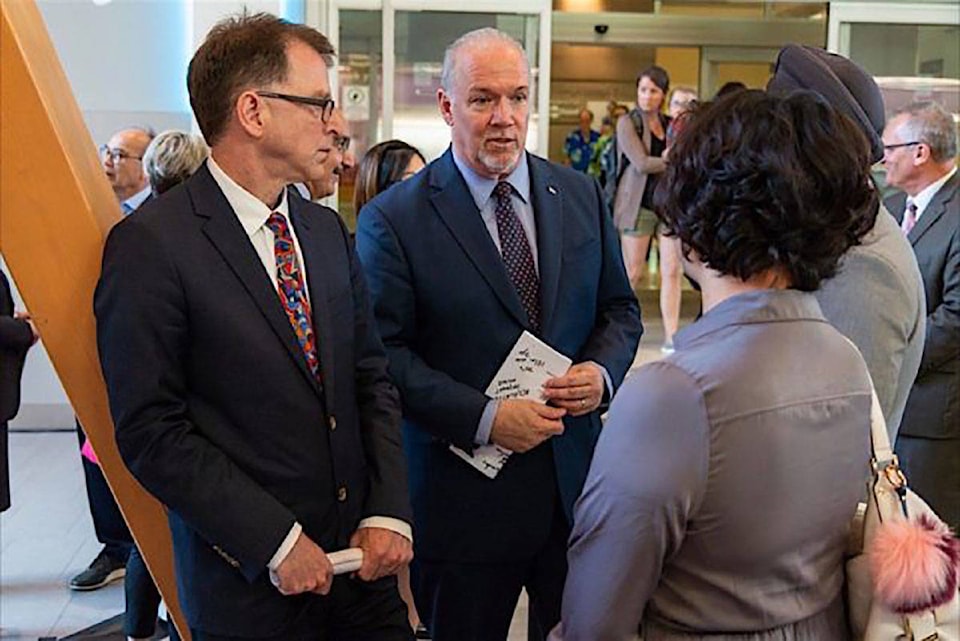The announced closure of Wheelhouse Integrative Medical’s walk-in clinic for Aug. 1 is the latest loss for health care services in Langford and surrounding centres; a region counting on service improvements by the Ministry of Health.
Roy and Rita Perren, 87 and 83, respectively, have seen Langford’s demand for health professionals swell since moving to a town of 6,000 in 1979. “We have had the same doctor – including his father – all that time,” Rita Perren wrote to the Goldstream Gazette.
Over the years, weekly blood level checks and monthly medication changes for chronic spinal stenosis were prescribed between the couple. The Perrens’ doctor, however, retired last January.
Left without a family physician and waiting for a promised replacement, the pair applied to be attached to Eagle Creek Medical Centre in View Royal. Rita said there are 1,200 applications ahead of them. What’s more, Roy’s pain medication can only be prescribed without a doctor through a walk-in clinic, after first obtaining medical records at a cost of more than $300, Rita explained.
“We have been told to go to (the emergency room), where we no doubt will get bumped time and time again for someone more serious,” she said. Their last emergency room wait was 10 hours overnight, a gruelling stay for Roy given his spinal condition. “We need a doctor desperately, but we are left high and dry … it has been a very stressful few months and no one is listening to us,” Rita wrote.
Dr. Vanessa Young, chair of the South Island Division of Family Practice and West Shore family doctor of 25 years, isn’t surprised to hear about the waitlist. Most West Shore doctors stopped keeping a waitlist due to the massive number of requests they receive daily, she said.
In 2016, the number of people in the western communities without a family doctor – known as attachment gap – was about 40,000 people, Young said. That gap for Greater Victoria is today approaching 100,000.
The Ministry of Health launched the Westshore Urgent Primary Care Centre on Goldstream Avenue in November 2018. The stated goal at the time was to attach 5,300 area residents with a family physician and narrow an attachment gap Mayor Stew Young estimated then to be 30,000.
RELATED STORY: 2018: Province announces new urgent care centre in Langford
The centre is today staffed with two physicians, two registered nurses, a mental health and substance use clinician and a social worker. But to date only 2,000 patients have been attached, to nurse practitioners working upstairs at St. Anthony’s Primary Care Clinic, according to Island Health. No explanation for the shortfall of 3,300 attachments was provided as of publication time.
Last September, the Ministry of Health committed to hiring 50 health professionals for the West Shore as part of their strategy to establish 39 primary care networks across the province. Those employed in the province’s primary care networks – from family doctors to social workers – will work across several sites in their regions.
To date, 24.5 professional care providers have been hired for the Western Communities Primary Care Network, said the Ministry of Health in an email. That includes 4.5 full-time equivalent family doctors, seven nurse practitioners, six social workers and six registered nurses.
While Vanessa Young appreciates a speedy hiring process, she said, “there’s actually a lot of learning for these professionals who’ve actually never worked directly in primary care before.” A staggered hiring approach is most practical, she added.
Health-care professionals already hired for the network account for 49 per cent of the total to be hired by 2024, and just 18 per cent of them are family doctors.
READ ALSO: Esquimalt’s temporary urgent and primary care centre to open Monday
Nevertheless, the addition of a mental health and substance abuse clinician one day a week “has made such a difference” in the quality of mental health care offered, Young said.
“To be able to refer patients in crisis to see an experienced professional to speak with them (and) brainstorm other resources if they’re needed – this is something we have been desperate for for many, many years,” she said.
The Practise Ready Assessment-British Columbia program has proven successful in improving South Island access to family doctors, Young added. Since 2015, the College of Physicians and Surgeons of B.C. has invited internationally educated family doctors to earn their provincial licence by serving communities in need.
“We’ve recently redefined communities of need so that urban and suburban communities could apply for these physicians,” Young said. She called the result – the hiring of 12 new doctors in Greater Victoria over the last two summers and possible placement of six more on the West Shore by September – “a huge success story.”
“By this fall and over the next year, that could account for 22,000 patients being attached (to a family doctor).”
Do you have a story tip? Email: kiernan.green@blackpress.ca.
Follow us on Twitter and Instagram,and like us on Facebook.